Vagus nerve stimulator

Should the medication treatment be ineffective or induce considerable side-effects then treatment with vagus nerve stimulation is considered. The precondition for this is that epilepsy surgery is not possible. The effectiveness of vagus stimulation is comparable to the use of other medications with however the advantage of a more favourable profile of side-effects.
What does a vagus nerve stimulator look like?
A vagus nerve stimulator ("Neurocybernetic Prosthesis" (NCP) – from the firm Cyberonics, Texas, USA) is a device consisting of a battery-powered pulse generator (5 cm diameter, 1 cm thick) and a cable with platin electrodes. It is implanted under the left collarbone and the electrodes are connected to the left vagus nerve, that is, the 10th cranial nerve, in the neck.
How is a vagus nerve stimulator implanted?
In contrast to epilepsy surgery, this is not an operation on the brain in the same sense. The vagus nerve stimulator is surgically implanted under general anaesthesia, an operation that takes around 1 to 11/2 hours. Two small incisions are made to the left armpit and to the left of the neck in order to bring the pulse generator and the electrodes into the correct the position. The functional operation of the stimulator is tested during the operation. A long hospital stay is not normally necessary after the operation.
How does the stimulation work?
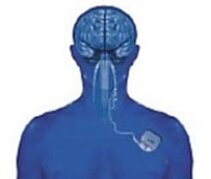
Weak electric signals are sent from the pulse generator at regular intervals (of normally 5 min.) to the electrodes and the vagus nerve and from there on to the brain. Stimulation is continued for about 30 seconds at a time. The doctor can programme both the stimulation interval and period according to individual requirements. After implantation the intensity of stimulation can be increased in the out-patient clinic on a monthly basis, depending on tolerance and effectiveness of the frequency of seizures. This adjustment is done by the doctor and is achieved by placing a special device over the skin above the location of the pulse generator. The life of the battery in the stimulator is about 4-5 years, and those in the new generation stimulators last about 7-8 years. A small surgical operation is needed to replace the battery.
Can you influence the stimulation yourself?
The stimulator can be influenced by you and not just by the doctor.
For this you will be given a magnet with which you can trigger an additional more intensive stimulation. By so doing you can try for instance to reduce the spreading of epileptic activity as the aura commences or your relatives can trigger a stimulation as soon as they see the early signs of a seizure.
By holding the magnet over the stimulator for a longer time you can inactivate it when for instance you do not wish to be disturbed by the impulses in particular situations.
Does vagus nerve stimulation really help against epileptic seizures?
The effectiveness of vagus nerve stimulation has been demonstrated in double-blind investigations in which different levels of stimulation intensity in patients with focal seizures were compared. Vagus nerve stimulation also appears to have a positive effect on patients with primary generalised seizures but the available data is less convincing in this case. Altogether 15000 patients have been treated to date with the vagus nerve stimulator, most of them in the USA. In Germany ca. 500 patients have received vagus nerve stimulation treatment.
Not all patients benefit from this treatment. While there is statistical proof of the effectiveness of this treatment it is, as with medication, not possible to know in advance whether vagus nerve stimulation will help individual patients. Seizure freedom will only be achieved in a few patients. A considerable reduction in seizure frequency is achieved in a third of the treated patients. Some patients also report a reduction in the intensity of the seizures. In some cases the success of the treatment can only be assessed after more than a year. A positive treatment effect appears to continue for a long time (years).
What are the side-effects of vagus nerve stimulation?
About half of the treated patients report hoarseness of the voice during the period of stimulation. This is normally not experienced as very bothersome; the stimulator can be temporarily inactivated when giving a talk or under similar circumstances (see above). Other side effects include discomfort or pain in the throat and difficulty swallowing.
On the whole, tolerance is good; in practice few patients wished the treatment to be terminated because of side-effects. An advantage of vagus nerve stimulation is that the combination with medications does not result in an increase in side-effects. Some studies report an enhancement in alertness and life quality when undergoing vagus nerve stimulation treatment. Negative effects on neuropsychological performance such as memory and language comprehension have not been found.
Should you consider vagus nerve stimulation?
Vagus nerve stimulation is a treatment option for you if your epilepsy can not be controlled by medication treatment and you are not suitable for epilepsy surgery. This has to be discussed with your treating doctor on an individual basis. Vagus nerve stimulation is not an option if you suffer from heart disease, dysphagia, lung disease, or have a stomach ulcer requiring treatment.
Practical points to consider:
- After implantation, MR imaging can only be performed with a special head coil. There is a risk of the body coil electrodes overheating. The magnet may not be taken into the room housing the MR scanner.
- When flying you should inform the security staff so that this is taken into account when screening for metal objects.
- Please note that the magnet can erase data on credit cards should it come within close vicinity of them.